
New heart procedure a life-saver
Valve replacement surgery performed at Promedica Toledo Hospital
9/10/2012
Heart valve replacement surgery patient Barbara Streight of Toledo walks with the aid of a walker to see Dr. Michael G. Moront.
The Blade/Amy E. Voigt
Buy This Image
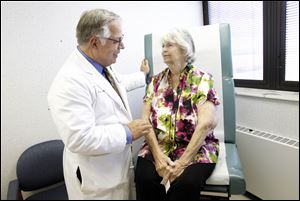
Dr. Michael G. Moront of Promedica Toledo Hospital goes through the first follow-up visit with heart valve replacement surgery patient Barbara Streight.
On her 81st birthday, Barbara Streight received a special gift: Her heart surgery at ProMedica Toledo Hospital was completed successfully within a few hours.
Three days later, Mrs. Streight was allowed to leave the hospital and return home because of her quick recovery.
"I am tired, but now I can breathe much better," Mrs. Streight told her cardiothoracic surgeon Dr. Michael Moront during her first follow-up examination a week later.
In January, the ProMedica Toledo Hospital was approved to perform transcatheter aortic valve replacement, a minimally invasive surgery that enables placement of a collapsible aortic heart valve into the body via the femoral artery in the thigh.
Mrs. Streight's was the sixth such surgery at the hospital since July. All the surgeries have been successful, according to Dr. Moront.
"I was glad that I was getting it done, because I was falling down on everything I did. I would work a little bit but then I had to rest. And my breath was so short," Mrs. Streight said. "I was not nervous at all. I trusted the doctors."
Mrs. Streight had a open-chest surgery in 2002. "I am still not over [the pain]," she said.
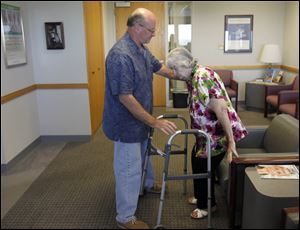
Barbara Streight is helped up by son Don Streight as she gets ready for her first follow-up visit.
But the valve replacement surgery was notably different. "That [open-chest surgery] was unbearable, but this [surgery] is much more tolerable," she said
Mrs. Streight first heard about the surgery from Dr. Moront, who suggested she do the testing to see if she would be a good candidate.
"They brought her back around 2010 and said 'Would you operate on her again?' When we looked at her, we didn't think that she would survive a surgery. Now we are able to do it this way, which is truly a revolution," Dr. Moront said.
Qualified patients include those who have severe symptomatic native aortic valve stenosis and have been determined inoperable for open aortic valve replacement by at least one cardiothoracic surgeon. They cannot have existing conditions that would preclude the expected benefit from correction of the aortic stenosis.
Dr. Moront said that about 25 percent of the people who go through the screening are good candidates.
"We evaluated about 65 to 70 people for the last eight months. We've done six. We are evaluating at least half a dozen," Dr. Moront said.
Almost 20 doctors, nurses, and supporting staff members were in the operating room when Mrs. Streight had her surgery.
In addition to Dr. Moront, the valve team included Dr. Robert Grande, a cardiologist, Dr. John Letcher and Dr. Fred Stockton, Dr. P. Kasi Ramanathan, interventional cardiologists and Dr. William Rachwal, another cardiothoracic surgeon. Erica Boonie, a registered nurse, is the valve clinic's clinical coordinator.
The hospital spent $3.2 million to build the new operating room and buy the equipment, according to Tedra White, a spokesman for the hospital.
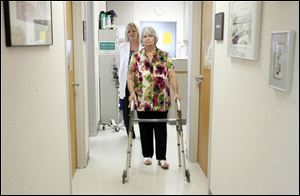
Heart valve replacement surgery patient Barbara Streight of Toledo walks with the aid of a walker to see Dr. Michael G. Moront.
The cost of the surgery is $60,000. The pre and post-operation fees depend on the patient's insurance coverage and vary from patient to patient. To be qualified for Medicare coverage, patients have to determined inoperable by two surgeons.
The valve for replacement was manufactured by Edwards Lifesciences LLC. On Nov. 2, 2011, the U.S. Food and Drug Administration approved the Edwards' Sapien Transcatheter Heart Valve as the first TAVR device for marketing in the country. The company only selected about 100 sites around the country for the surgery, according to Dr. Moront.
Dave Ollio, an area sales representative of Edwards, said that the company considers four factors to determine if a site is a good candidate: a comprehensive valve team, strong administrative support, multidisciplinary approach by valve clinic, and sufficient facilities.
"We were pretty confident in the surgery. When they decided that mom can get this procedure done, we were thrilled. It seemed so simple," said Mrs. Streight's son Don Streight, 60, of Curtice, Ohio. "[The doctors] said that in the condition that she was in, she maybe could make it two years. Hopefully this will give her quite a few more."
The second patient, Walter Yeager of Toledo, had his surgery in July and has recovered well. Mr. Yeager, 82, said he would highly recommend the surgery to other candidates.
"I am feeling good now. I feel like I won a lottery in the medical world. I want to thank everyone behind the scene. I wouldn't be here if there were not persistence of Dr. Grande and Erica," Mr. Yeager said.
"This opens up a therapy to patients who in the past would have spent the last years of their life in the hospital," Dr. Moront said.