
New-to-St. Vincent’s technique halts nurse’s aneurysm
12/11/2012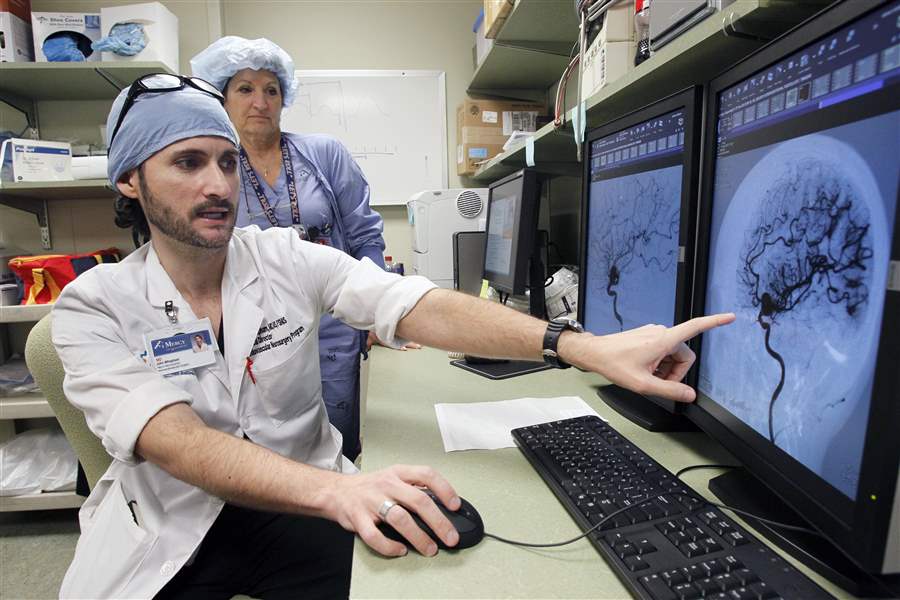
Dr. John Whapham, a neuroendovascular surgeon, describes the aneurysm coiling procedure performed on Olivia Cox, behind him.
The Blade/Dave Zapotosky
Buy This Image

Surgical nurse Olivia Cox is back on the job. A casual conversation with a vascular surgeon led to discovery of her cerebral aneurysm.
It started with a headache and pain in Olivia Cox’s shoulder, arm, and back.
Mrs. Cox, a longtime surgical nurse at Mercy St. Vincent Medical Center, continued to work despite a painful case of shingles, and she mentioned her symptoms in a casual operating-room conversation with Dr. Paul Clark, a vascular surgeon.
The discussion took place in late September, and it sparked the discovery of a large cerebral aneurysm behind Mrs. Cox’s left eye. A Nov. 27 procedure took place at St. Vincent, where the minimally invasive technique used is so new to the hospital that Mrs. Cox didn’t know about it until she needed it.
The diagnosis and treatment involved numerous St. Vincent physicians, nurses, and others, several of whom she saw again Monday when she returned to work for the first time since the procedure.
“I was very lucky,” said Mrs. Cox, 58, of Petersburg, Mich. Her colleagues call her Lea.
Trim, energetic, and dressed head to toe in hospital blue, Mrs. Cox gave no visible indication she had spent five hours recently undergoing a coiling procedure to treat an aneurysm that measured just shy of the size of a quarter and dwarfed a more typical pea-sized aneurysm.
It started with a headache and some left-side pain.
Mrs. Cox wasn’t too concerned about shingles. She figured: “You get old, and stuff starts hurting, and, you know, you still go to work.” When she told Dr. Clark about her symptoms, he advised her to look into it.
“I thought it might be something else,” Dr. Clark said.
Dr. John Whapham, a neuroendovascular surgeon, describes the aneurysm coiling procedure performed on Olivia Cox, behind him.
It was a passing conversation, but he said he took it seriously because she didn’t look well, and he hadn’t heard her talk about headaches before. Mrs. Cox said Dr. Clark’s office arranged for an appointment with Dr. Ahmed Arshad, a neurologist, who ordered an MRI.
“If Dr. Clark’s office had not gotten me that appointment I probably would have had a rough time getting in to see a neurologist ’cause they are so busy,” she said.
Had it not been for that appointment, she acknowledged, she might have thought: “I’m a nurse. I can take care of myself.”
The images revealed the sinister-looking spot. Enter the next physicians: Dr. John Whapham, a neuroendovascular surgeon, who along with the center’s chief of neurosurgery, Dr. Michael Healy, arranged for the coiling procedure, which is fairly new to St. Vincent. It can be used in some cases instead of a craniotomy, during which the neck of an aneurysm is clipped to stop blood flow to prevent rupturing.
The coiling option offers a minimally invasive procedure using a catheter placed in the leg’s femoral artery. The physician uses images to guide the way to the brain, where thin coils made of nickel, titanium, and platinum are released to pack the aneurysm and block blood flow. Dr. Whapham estimated he used about 50 feet of coil, “framing in the aneurysm” like a ball of yarn. Dr. Healy was at the ready throughout the procedure in case surgery was required. The coils remain inside Mrs. Cox.
The coiling procedure has been performed a handful of times at St. Vincent so far this fall under Dr. Whapham, who came to the hospital in July from Loyola University Medical Center to build a comprehensive stroke program.
“This was a big thing bringing this program to St. Vincent’s. A lot of people were involved in it,” Mrs. Cox said about the new offering that allowed her to undergo the procedure close to home.
Dr. Whapham flipped through images of her procedure, illustrating how the aneurysm was treated and describing the planning, measuring, and three-dimensional modeling technology that helped determine she was a good candidate for the procedure.
The recovery period after coiling is shorter than that for traditional surgery techniques, he said. Mrs. Cox left the hospital the day after the procedure and returned to work about two weeks later, grateful for the help and expertise.
The shingles could be connected to aneurysm and “may have been the only tell-tale symptom” leading to the discovery by doctors, Dr. Whapham said.
“That may have saved her life,” he said.
Dr. Clark spent part of Monday working in the operating room alongside her. He’s retiring this week and called Mrs. Cox, who has worked at St. Vincent for 37 years, a “treasure.” He welcomed her return to the hospital as a nurse instead of a patient.
“I wasn’t sure she had [the procedure] done yet. She looked too good,” Dr. Clark said. “It’s nice to see a friend get better.”
Contact Vanessa McCray at: vmccray@theblade.com or 419-724-6065.