
COMMENTARY
Opiate epidemic exacts deadly toll across Ohio
Time to find, enact remedies is now
2/16/2014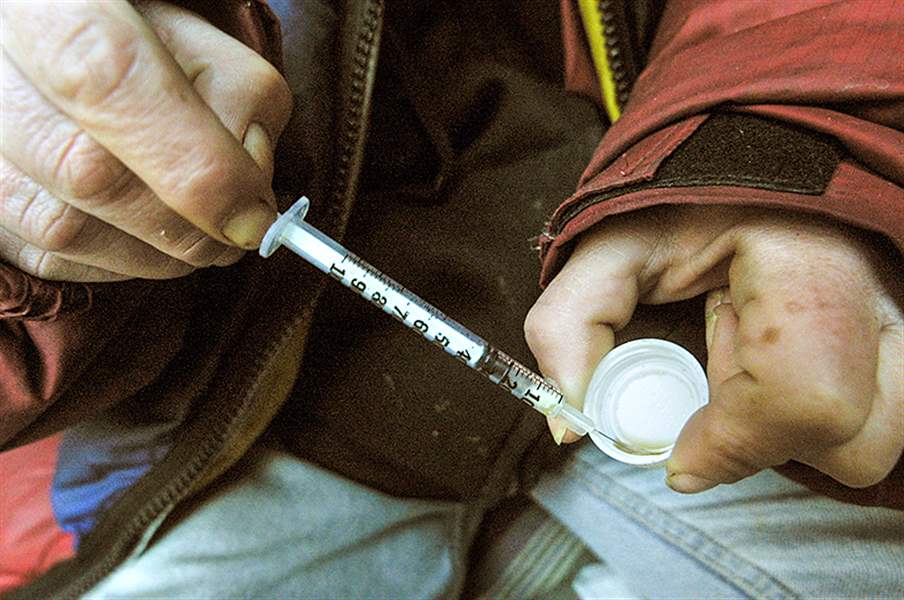
People hooked on prescription painkillers, such as Vicodin, can feed their opiate addiction more easily and more cheaply by moving on to heroin.
GETTY IMAGES

Jeff Gerritt
Opiate addiction can start with a single white pill that sends the user into euphoria, but soon replaces fleeting bliss with a solitary, unquenchable thirst.
Needing more and more of the drug just to feel normal, users can move within months from prescription painkillers such as Vicodin to heroin, feeding their addictions more cheaply, more easily — and more lethally.
An opiate epidemic is killing 22 Ohioans a week. In northwest Ohio, the number of heroin-related deaths more than doubled last year, to 80 from 31 in 2012.
None of those deaths got the attention and hype that surrounded the fatal heroin overdose of actor Philip Seymour Hoffman two weeks ago. Still, for their family and friends, the hole left was just as big, the pain equally deep. Opiates, including heroin, have thrust the agony of addiction on 200,000 Ohioans, a population as large as most of Toledo.
The Blade’s Pages of Opinion start a series on Ohio’s opiate epidemic today. Running throughout the year, “Prescription: Addiction” will examine the problem from the ground level. It will prescribe policies and programs to reduce drug abuse and deaths and treat the addicted.
Opiate addiction touches people everywhere — now more than ever before. Most victims of heroin-related deaths in Lucas County last year were middle-aged, suffered from chronic pain, and had graduated to heroin from prescription painkillers.
Ten years ago, I spent five days with a recovering heroin addict in a Detroit rehabilitation center — one of the many addicts I’ve talked to over the years. A heating/ventilation repair worker, he started his opiate habit by rifling through home medicine cabinets, looking for prescription painkillers. After a year or so, he graduated to heroin.
Like a lot of other addicts, he lost everything. He checked into rehab on a rainy spring morning with only the clothes on his back. Among his peers, some were lucky enough to hold onto their jobs, homes, and families, but even they had lost control of their lives.
In treatment, he could, for the first time in years, tell his story openly and without fear, and even laugh about it. When he started using, it was all fun and no problems, but the drugs soon became all problems and no fun. Addiction took him to a cold dark spot from which there seemed no way out.

I saw him for the last time the day after he was released from rehab, waiting at a bus depot, on his way to his sister’s house in North Carolina. I hope he made it.
In Ohio today, opiate abuse is an even bigger problem than it was in Michigan a decade ago. Ohio has the nation’s 12th highest drug overdose mortality rate, with 16 people per 100,000 dying of overdoses every year, according to a report by the nonprofit Trust for America’s Health.
Drug abuse often breeds social hysteria. We don’t want to start a witch hunt against prescription painkillers, which have promoted treatment and alleviated a lot of unnecessary suffering for many people, including cancer patients.
Making these drugs inaccessible by overregulating them would be a mistake. But we do want policies and programs, including better-educated physicians, that deal with their potential for abuse and addiction. Chemically, painkillers are not much different from heroin, which is as much as 10 times cheaper than pills.
Today’s editorial (Page B4) looks at how well-meaning physicians have unwittingly helped to create Ohio’s opiate epidemic. I talked to an orthopedic surgeon from Columbus whose license was suspended for six months last year. He wasn’t running a pill mill. Nor did he seek to make money or hurt people.
Still, he knew nothing about the dynamics of addiction. Now he knows he was part of the problem and, hoping to educate others, is bravely speaking up.
He’s not alone in overprescribing. The amount of opiates prescribed in Ohio has increased ninefold since the late 1990s. Today, enough pills are dispensed to give every man, woman, and child in the state nearly 70 doses a year.
In a generation, we’ve gone from a society that sharply restricts painkillers to one that routinely dispenses them for dental work, migraines, and backaches, usually without warning. Two months ago, I was prescribed 15 Vicodins for a root canal that gave me only mild discomfort.
Education and treatment, although imperfect, remain the most effective remedies. No doubt, some people won’t listen even to the best information. And treatment programs can fail, and fail. I’ve met people who have gone through rehab seven or eight times.
Eventually, though, they made it out. It’s not good ever to give up on people, especially when the alternative is throwing more drug users into prison, where they get no help and cost taxpayers $30,000 a year each.
Few people in Ohio have not felt this problem, directly or indirectly. We hope this series will give them a broader and deeper understanding of an epidemic that has touched so many of their families and communities. Most of all, we hope to make a difference.
Jeff Gerritt is The Blade's deputy editorial page editor.
Contact him at: jgerritt@theblade.com, 419-724-6467, or follow him on Twitter @jeffgerritt.