
Experimental surgery for unusual form of infertility produces a baby boy
10/7/2013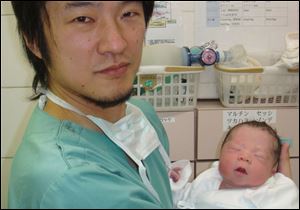
Dr. Kazuhiro Kawamura holds a newborn baby whose 30-year-old mother was treated for primary ovarian insufficiency, sometimes called premature menopause.
NEW YORK — A 30-year-old infertile woman gave birth after surgeons removed her ovaries and reimplanted tissue they treated in a lab, researchers report.
The experimental technique was only tried in a small group of Japanese women with a specific kind of infertility problem, but scientists hope it can also help women in their early 40s who have trouble getting pregnant because of their age.
The new mother gave birth to a son in Tokyo last December, and she and the child continue to be healthy, said Dr. Kazuhiro Kawamura of the St. Marianna University School of Medicine in Kawasaki, Japan. He and others describe the technique in a report published online Monday by the Proceedings of the National Academy of Sciences.
The mother, who was not identified, had been diagnosed with primary ovarian insufficiency, an uncommon form of infertility sometimes called premature menopause. It appears in about 1 percent of women of childbearing age. The cause of most cases is unknown, but the outcome is that the ovary has trouble producing eggs.
That leaves women with only a 5 percent to 10 percent chance of having a baby unless they get treated. The standard treatment is using donor eggs.
After the experimental procedure, Kawamura and colleagues were able to recover eggs from five of their 27 patients. One woman went on to have a miscarriage, one did not get pregnant, and two more have not yet attempted pregnancy, Kawamura said in an email.
The approach differs from what has been done to preserve fertility in some cancer patients, who had normal ovarian tissue removed and stored while they underwent cancer treatments, and then put back. The new work involved ovaries that were failing to function normally.
In the ovary, eggs mature in structures called follicles. For women with the condition the new study targeted, the follicles are either missing or failing to produce eggs. The experimental treatment was designed to stimulate dormant follicles.
First, the women’s ovaries were removed and cut into strips, which were frozen. Later the strips were thawed and cut into tiny cubes, a step intended to stimulate maturation of the follicles. Then the cubes were treated with drugs to stimulate further development of the follicles. Cubes were then transplanted just under the surface of the women’s fallopian tubes.
Within six months, eight women showed signs of follicle maturation, and five of them produced eggs for fertilization in the lab with their husbands’ sperm.
The fertilized eggs were grown into early embryos, which were frozen for preservation. In the three attempts at pregnancy, one or two embryos were implanted in the women.
The researchers found that half the 27 patients had no follicles at all, which meant the treatment could not help them, said Aaron Hsueh of Stanford University, senior author of the study.
He also said researchers hope to find a way to stimulate follicles without removing the ovaries.
Dr. Sherman Silber of the Infertility Center of St. Louis criticized the approach, saying he has had success by using drugs rather than surgery to treat the condition.
He also disagreed with the researchers’ explanation for why their treatment worked.
Some other experts said treatment with drugs often does not work.
The new results, experts cautioned, must be viewed as preliminary.
“It shows a lot of promise (but) I don’t think it’s even close to being ready” for routine use, said Dr. Mark Sauer of the Columbia University Medical Center in New York. Dr. Amber Cooper of Washington University in St. Louis called the technique “very much an experimental method.”
The reported efficiency is very low, and the possible health risk to babies born from the method is unknown, said David Albertini of the University of Kansas Medical Center.
“One success does not mean we have a treatment.... Stay tuned,” he said.