
NOT WHAT THE DOCTOR ORDERED
Delays, denials thwart patients hoping for help
Insurers’ rules trump doctors’ orders, even in dire scenarios
8/25/2008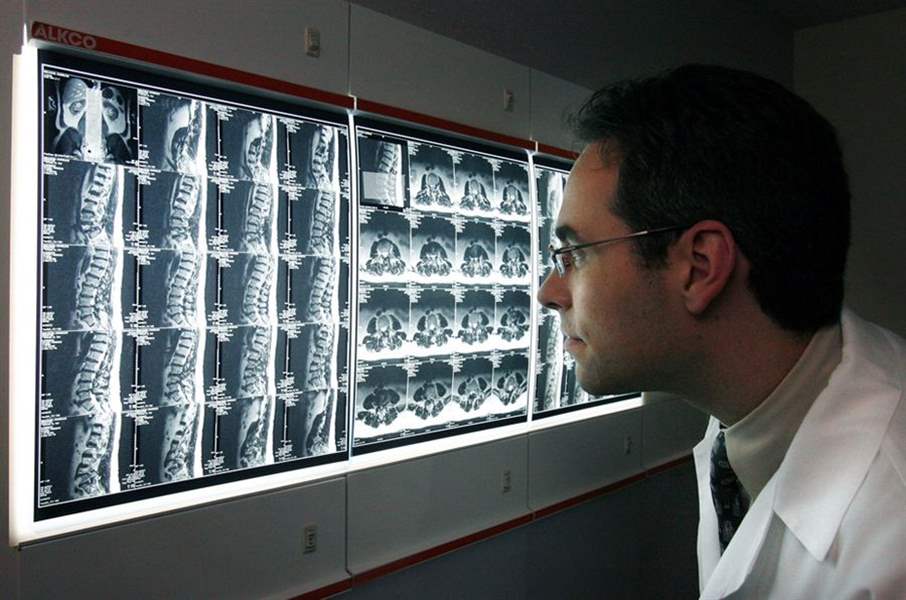
Dr. David Hart, who operated on Mr. Hodnik, says he is frustrated that insurers are blocking patients from undergoing new procedures.
THE BLADE/JEREMY WADSWORTH
Buy This Image
Second of four parts.
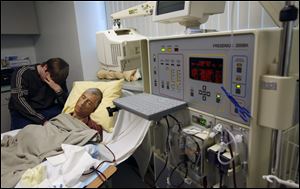
Randy Steele undergoes dialysis while his son, Jonathon, sits with him. Mr. Steele waited weeks to learn that his insurer would pay for an out-of-network, second evaluation to determine whether he was a candidate for a potentially life-saving kidney-liver transplant.
OAK HARBOR, Ohio -- Randy Steele was running out of options.
Mr. Steele, 64, of Oak Harbor shuffled back and forth between hospitals in northern Ohio last year as physicians scrambled to stay ahead of the hepatitis C virus invading his body and slowly threatening his liver and kidneys.
His prognosis seemed grim.
He was referred to the renowned specialists of the Cleveland Clinic to offer him a second opinion on a potentially life-saving kidney-liver transplant.
Cleveland Clinic quickly fit Mr. Steele onto its schedule. But instead, his appointment was canceled and he waited weeks to learn if his insurer would pay for his evaluation at the clinic, which was outside the network for his health plan.
“I truly believe that Randy could have been helped,” Mr. Steele’s wife, Pam, told The Blade.
Mr. Steele, like many patients across the country, was the victim of a complex health-care bureaucracy and an insurance industry that repeatedly denies doctors’ orders - leaving patients bewildered and suffering.
Others such as Bill Hodnik, 41, endured the same shortcomings.
He suffered months of pain while his insurer delayed and denied coverage for a surgery ordered by his physician.
READ THE SERIES: Not What The Doctor Ordered
A herniated disc in Mr. Hodnik’s neck sent numbing shivers down his left arm, rendering it useless. For years, back problems bothered Mr. Hodnik, a factory worker living in suburban Cleveland, but last year the pain intensified.
Mr. Hodnik’s physician told him the optimal solution to his problems would be cutting-edge artificial disc replacement surgery, rather than a more traditional spinal-fusion operation, which sometimes leads to additional operations.
“We don’t know how long we are going to live or what I am going to be like in 40 years, but he said the artificial disc was a much better choice than the fusion, and it would be a lot better for you in the long
run,” Mr. Hodnik said. “I was all for it.”
The surgery was scheduled, but he never underwent the procedure. After months of repeated delays and denials from his insurer, and with his disability insurance running out, Mr. Hodnik needed to return to work, and so - against doctor’s orders - he settled on fusion surgery.
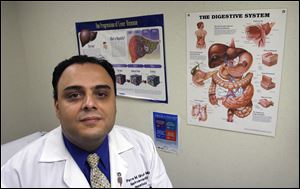
Dr. Pierre Gholam of Cleveland’s University Hospitals Case Medical Center referred Mr. Steele to the Cleveland Clinic for a second opinion with the hope that the clinic could overcome complications presented by the patient’s weakened heart and perform a transplant.
An emerging crisis
A Blade investigation shows that doctors nationwide believe there is an emerging crisis in providing health care to their patients because insurers routinely challenge their orders.
The investigation included interviews with about 100 physicians and an online survey of members of the Ohio State Medical Association and American Medical Association. The Blade prepared the survey questions, which the associations sent to their members.
Of the 920 respondents, more than 99 percent said insurers had interfered with their clinical decisions.
Doctors said patients usually receive the therapy, testing, medication, or procedure prescribed for them. But too often, physicians said, there’s a lapse in time between the office visit and when the care or test is delivered because of interference by insurers.
And 14 percent of the respondents to the nonscientific survey said they have had a patient seriously injured or harmed because of interference with their clinical decisions.
A grim prognosis
Randy and Pam Steele live on two acres in Ottawa County, a 45-minute drive from Toledo. Their home is brightened by four children and three dogs roaming about the house and yard.
The Steeles, who homeschool their children, have a classroom on the main floor of their home that converts into a hospital ward for Mr. Steele when he is too sick to walk upstairs.
The Steeles have a big family, with 11 children, all from past marriages or through adoptions. Of the 11, seven are grown - including adopted triplets and three sons who have served in the U.S. military in the Middle East, with two in Iraq.
Four of the children live at the Steeles’ house in Oak Harbor, including Thomas and Brandon, who are foster children, and Celeste, an adopted child from Mexico.
A former Mormon minister in Lima, Ohio, Mr. Steele received his master’s degree in engineering from Ohio State University in 1973. During his engineering career, Mr. Steele helped BP set its safety specifications.
Mr. Steele, later an engineer at the Sunoco Toledo Refinery, has battled illness since childhood. He suffered with rheumatic fever in his youth, and the fever affected his heart, requiring valve-replacement operations in the late 1960s and again in the 1980s.
In 2001, doctors diagnosed Mr. Steele with hepatitis C, an often-deadly disease that destroys the patient’s liver. Mr. Steele likely contracted the virus through a tainted blood transfusion he received during his first heart-valve replacement operation, when blood wasn’t routinely tested.
Under treatment for hepatitis C, Mr. Steele worked until September, 2006, when he became too ill to continue.
Mr. Steele has spent much of the past two years in hospitals or tethered to dialysis machines, defying predictions of his death, or prognoses that he would never walk again or would survive only in a vegetative state.
In July, 2007, Mr. Steele spent weeks in intensive care with his kidneys failing at the University of Toledo Medical Center, formerly known as the Medical College of Ohio hospital.
Mrs. Steele said a doctor and a social worker at the hospital told her that her husband’s insurer, Medical Mutual of Ohio, was pressuring the hospital to discharge her husband as his medical bills mounted.
Paula Sauer, vice president of care management for Medical Mutual, said the entire stay at University of Toledo Medical was approved and she couldn’t comment on what hospital personnel specifically told Mrs. Steele.
“There’s no reason that anybody should be told that the insurer is kicking the [patient] out,” Ms. Sauer said. “The physician needs to make his medical and legal, ethical, clinical decision and follow what he is liable for. I’m not sure why they felt this way.”
Within a few days of Mr. Steele leaving the hospital, his kidneys shut down, indefinitely landing him on dialysis treatments three times each week.
He quickly returned to the University of Toledo Medical Center and later to University Hospitals Case Medical Center in Cleveland, where he was evaluated for a kidney-liver transplant.
If successful, a transplant could have extended Mr. Steele’s life, but without the transplant, doctors told him he had weeks or months to live.

Nine months after receiving a grim prognosis, Randy Steele is alive and savoring each moment. He marked July 4 by taking in a Mud Hens game, where he got a push from his son, Jonathon.
A second opinion?
After examining Mr. Steele, University Hospitals’ transplant team reported that it couldn’t offer him a kidney-liver transplant because of concerns that his damaged heart would diminish the likelihood he would survive the operation and thrive afterward, said Dr. Pierre Gholam, a transplant specialist.
Dr. Gholam referred Mr. Steele to the Cleveland Clinic for a second opinion with the hope that the clinic, with its expert cardiovascular care, could overcome the complications presented by his weakened heart and perform a transplant.
Dr. Gholam told The Blade that he recalled telling the Steeles that “even though our assessment here is that we don’t feel we can do this in a way that’s safe for him, the Cleveland Clinic has a pretty renowned cardiothoracic and cardiovascular program and perhaps they can offer him additional things that we may not be able to offer him.”
He added, “I wasn’t certain that was the case, but I thought he was someone that had a good quality of life who certainly had a family that wanted him to be around and have additional quantity of life.”
Dr. Gholam wasn’t overly optimistic the Cleveland Clinic would be able to offer Mr. Steele a transplant. “But for his peace of mind and for the peace of mind of his wife, I think he needed to hear that and he needed to have a second shot at this, which was legitimate,” the transplant specialist said.
Cleveland Clinic placed Mr. Steele on its schedule to begin his evaluation for a kidney-liver transplant Sept. 27, 2007. But two days before the appointment, the Cleveland Clinic notified Mr. Steele that Medical Mutual wouldn’t cover his second opinion because the clinic isn’t part of his health plan’s network.
Mr. Steele’s doctor quickly wrote a letter to Medical Mutual explaining why Mr. Steele should be covered for the consultation with Cleveland Clinic.
Medical Mutual’s Ms. Sauer told The Blade that Mr. Steele’s second opinion was approved for coverage the same day he was to meet with the transplant team at the Cleveland Clinic. The next day, she said, Medical Mutual mailed a letter to the Steeles notifying them of the decision.
But the letter states: “All services should be performed within the network.”
The letter continued, “Please be advised that utilizing a provider outside of the network/first tier may result in additional financial liability and if you use a non-contracting provider, you may be financially responsible for the difference between the provider’s charged amount and the contractual amount.”
The letter, which was copied to the Cleveland Clinic and Mr. Steele’s primary care physician, not Dr. Gholam, directed the patient to customer service for questions.
For Mrs. Steele, the letter raised more questions than answers, so she called Medical Mutual to find out more.
“When I called Medical Mutual, they said that Cleveland Clinic was not in the network for our policy. I did call to check it because it was so important,” Mrs. Steele said, adding, “Knowing just a basic transplant for Randy would be $500,000, there would be no way I could handle the liability.”
Mrs. Steele, frustration growing, e-mailed friends and family.
“We still have not been able to go to Cleveland Clinic although they wanted to see us last week,” Mrs. Steele wrote on Sept. 30. “We continue to pray that God opens a door. Our transplant team from [University Hospitals] has challenged the medical insurance company and only time will tell.”
A week later, on Oct. 8, Mrs. Steele wrote again, enlisting friends and family members to seek intervention by state and federal lawmakers, including U.S. Rep. Marcy Kaptur (D., Toledo). A family friend scripted a template for a letter-writing campaign to officeholders and the media.
“The family is suffering a dangerous waiting game because of the bureaucracy of their HMO,” the form letter stated. “This seems to be a case of bureaucrats [not his medical team] making a decision on whether to operate on a man when he has no time for games.”
On Oct. 9, Cleveland Clinic learned by phone that Medical Mutual would cover Mr. Steele’s second opinion, clinic spokesman Heather Phillips said. The clinic again fit Mr. Steele into its schedule, this time for the week of Oct. 22 - nearly a month after his original appointment.

Mr. Steele and his wife, Pam, pray during a Christmas service at a Port Clinton church.
A disappointing process
As Dr. Gholam feared, Mr. Steele’s visit to Cleveland Clinic yielded no life-saving answers.
After weeks of testing, a team of specialists determined Mr. Steele would not be a candidate for the transplant because he had too many factors working against him. The clinic’s team didn’t believe the lag between his initial appointment and his actual evaluation made a difference in Mr. Steele’s final determination, Ms. Phillips said.But the Steeles still wonder if the results would have been different had her husband been able to keep his original appointment.
“I felt like I was being cheated an opportunity of being able to determine if I was going to be able to have a transplant or not,” Mr. Steele said.
Mrs. Steele fears her husband’s insurance plan worked against him when he needed it most.
“I truly believe the insurance companies have created a situation that has not been in Randy’s best interest,” she said.
A painful experience
Like millions of Americans, Bill Hodnik is no stranger to back pain.
His father and sister both underwent lower back operations. In the late 1990s, a doctor diagnosed Mr. Hodnik with degenerative disc disease, which commonly causes neck and back pain.
By March, 2007, Mr. Hodnik’s lower back condition worsened to the point that his left leg went numb and he was transported by ambulance to the hospital, where Dr. David Hart, the director of the Neurosurgery Spine Center of the Neurological Institute of University Hospitals Case Medical Center, performed surgery to clean up a herniated disc in his lower back in May.
“Over the course of my life, probably playing softball, bowling, working, I herniated a disc,” Mr. Hodnik said.
A few months later, after returning to work, Mr. Hodnik began feeling numbness and slight pain in his neck and shoulder. He assumed he had pulled a muscle in his shoulder and treated his discomfort with over-the-counter pain medication.
“One day, the numbness just went right down my arm,” said Mr. Hodnik, who returned to Dr. Hart’s office, this time with neck pain and numbness. Magnetic resonance imaging soon showed that a herniated disc was pushing up against Mr. Hodnik’s spinal cord, causing his arm to go numb.
In the past, Mr. Hodnik’s condition would be addressed with a spinal fusion surgery, an operation in which two or more vertebrae are fused together. The operation has its drawbacks, especially for young patients, because it places pressure on surrounding discs, sometimes requiring follow-up procedures.
Considering his age and overall good health, Mr. Hodnik said Dr. Hart told him he would be an ideal candidate to have an operation to replace his herniated disc with an artificial cervical disc, approved by the Food and Drug Administration in July, 2007. The FDA began approving artificial discs for other parts of the back in 2004.
“This is a revolutionary kind of technology that allows a person to avoid having their spine fused, instead having essentially a mechanical disc placed,” Dr. Hart said.
“What we used to do ... [is] fuse the vertebrae together. That has significant consequences for the patient both in the long term and the short term.”
Mr. Hodnik was scheduled for artificial disc replacement surgery on Oct. 24, but the night before the operation, he heard from the hospital that the surgery couldn’t be performed because his insurer wouldn’t approve it.
A week later, Mr. Hodnik received a notice in the mail from his insurer, UnitedHealth Group Inc., stating that the surgery wasn’t covered because of a lack of study to prove its merits.
‘The jury is still out’
UnitedHealth, the nation’s largest insurer, declined to comment on why it rejected the doctor’s recommendation for Mr. Hodnik’s surgery, saying it does not comment on specific patient cases.
Generally, though, the company doesn’t cover unproven services, such as disc replacement surgery, said Dr. Dick Justman, UnitedHealth’s national medical director.
So far, studies comparing disc replacement and fusion surgeries have been among small groups of patients, and researchers have only looked at results after two years, Dr. Justman said. More evidence about disc replacement is needed to ensure it is a good alternative to fusion surgery, which does have drawbacks, he said.
“We will be very happy to see any alternative to [fusion] surgery come forward,” Dr. Justman said.
“In a situation such as this, the jury is still out,” he added. “The studies are simply too small, and they have not gone out far enough. We are eager to see this research go out a few more years.”

Bill Hodnik of suburban Cleveland had spinal-fusion surgery after his insurer rejected a federally-approved artificial disc replacement favored by his doctor.
The jury is still out
UnitedHealth, the nation's largest insurer, declined to comment on why it rejected the doctor's recommendation for Mr. Hodnik's surgery, saying it does not comment on specific patient cases.
Generally, though, the company doesn't cover unproven services, such as disc replacement surgery, said Dr. Dick Justman, UnitedHealth's national medical director.
So far, studies comparing disc replacement and fusion surgeries have been among small groups of patients, and researchers have only looked at results after two years, Dr.
Justman said. More evidence about disc replacement is needed to ensure it is a good alternative to fusion surgery, which does have drawbacks, he said.
We will be very happy to see any alternative to [fusion] surgery come forward, Dr. Justman said.
In a situation such as this, the jury is still out, he added. The studies are simply too small, and they have not gone out far enough. We are eager to see this research go out a few more years.
A denial of treatment
In mid-November, Dr. Hart appealed UnitedHealth’s initial decision with hopes of getting a prompt final resolution for Mr. Hodnik. But the process dragged on for two more months as Mr. Hodnik struggled to get a final answer from his insurer.
In the meantime, Mr. Hodnik’s disability insurance was running out and the constant pain was taking a toll on his marriage and his family. Mr. Hodnik has two young children - a 4-year-old and a 2-year-old.
“Imagine taking care of those two with no use of your left arm, being in pain, and you can’t sleep,” Mr. Hodnik said.
“Did it put a strain on the family? Yeah it did. It put a lot of strain between me and my wife. I don’t mind taking care of the kids, but when you have no use of your left arm, you are taking pain medication just so you can move your arm a little bit, but you still can’t play with your kids.”
By January, Mr. Hodnik said he called UnitedHealth about every other day to check on his appeal, often hearing contradicting reports on its status, including once mistakenly being told he was approved for surgery.
Finally, in mid-January, he received his last denial. Needing to return to work, he decided not to pursue his appeal further and opted for the fusion surgery.
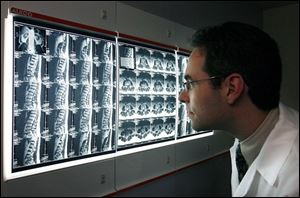
Dr. David Hart, who operated on Mr. Hodnik, says he is frustrated that insurers are blocking patients from undergoing new procedures.
It's annoying
Dr. Hart, who performed the surgery, said he is frustrated that many insurers are blocking patients from undergoing newly conceived procedures, like disc replacements, that can help them.
“Every study has shown that these artificial discs are as good as or better than a fusion in terms of patient outcomes, patient satisfaction, return to work status, and all of these things that have big societal impact,” Dr. Hart said.
Mr. Hodnik’s fusion surgery went smoothly, he’s returned to work, and he can enjoy summertime activities with his family.
He doesn’t know what the future holds for his back, but Mr. Hodnik isn’t angry at his insurer.
“If they would have come out and said Dec. 1 it was denied [because of lack of study], we could have gone on and had the fusion done and I could have been back to work at the end of January,” Mr. Hodnik said.
Not being able to get what he wants for his patients is difficult for Dr. Hart to accept.
“For me, it’s an inconvenience, it’s a frustration, it’s annoying, it’s insulting, and as a doctor who has great concern and care for my patients, it upsets me. In the end, it doesn’t truly affect me personally ... But good lord, it has a huge impact on my patients,” Dr. Hart said.
Lost opportunities
Nine months after his doctors said he was terminally ill with little time left, Randy Steele is still alive and savoring each moment with his family.
His health - bolstered by dialysis sessions every Tuesday, Thursday, and Saturday at Maumee Bay Dialysis Center in Oregon - is stable.
Last month Mr. Steele underwent surgery to replace his implanted defibrillator, a device that helps his heart beat properly.
In the months since doctors gave Mr. Steele little time to live, he celebrated his 16th wedding anniversary with his wife and his 64th birthday which coincided with Father’s Day, and he attended a Toledo Mud Hens baseball game on the Fourth of July.
“Each day is a gift and a miracle,” Mrs. Steele said.
The Steeles now say they are left to wonder if insurance delays squandered Mr. Steele’s chance for more days.
But still, Mr. Steele says he holds no grudges against Medical Mutual, but his concerns about the role of insurers in health care linger.
“Sometimes it just interferes with patients’ lives and that upsets me because it is interfering with my life,” Mr. Steele said. “I had some opportunities, maybe for transplants, that are gone and they are not ever going to be able to be replaced.”
Contact Steve Eder at: seder@theblade.com or 419-304-1680.